Priority Issues
Other Issues
-

2030 Seismic Requirements
-

Affordability
-

Ambulance Patient Offload Time
-

Behavioral Health
-

Clinical Care
-

Continuum of Care
-

Coverage
-
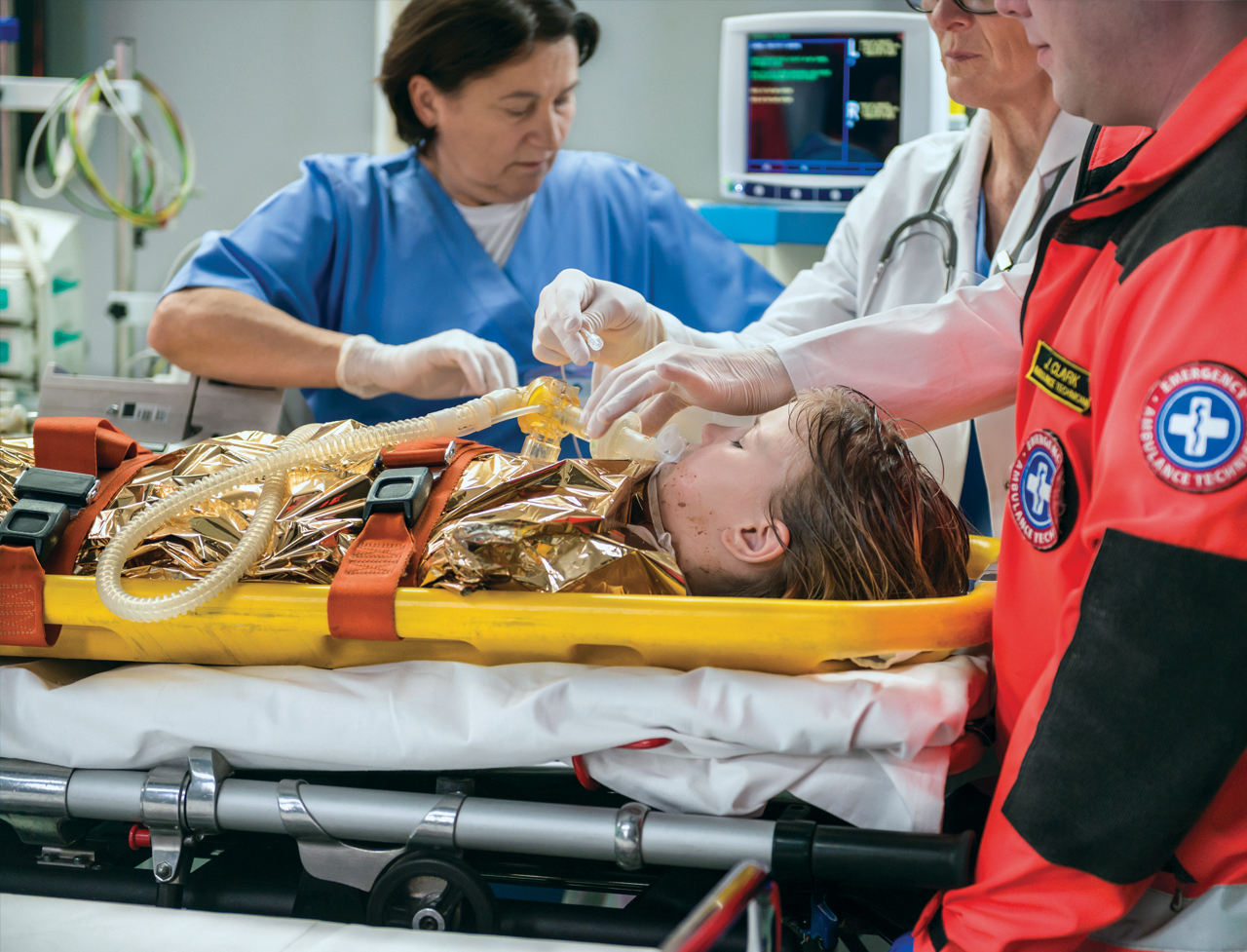
Emergency Department/Trauma
-

Emergency Preparedness
-

Finance & Reimbursement
-

Health Care Partnerships
-

Health Equity
-

Health Information Management & Technology
-

Holding Insurers Accountable
-

Hospital Operations
-

Laws & Regulations
-

Licensing & Accreditation
-

Medi-Cal
-

Medicare
-

Minimum Wage
-

Prescription Drug Pricing
-

Price Transparency
-
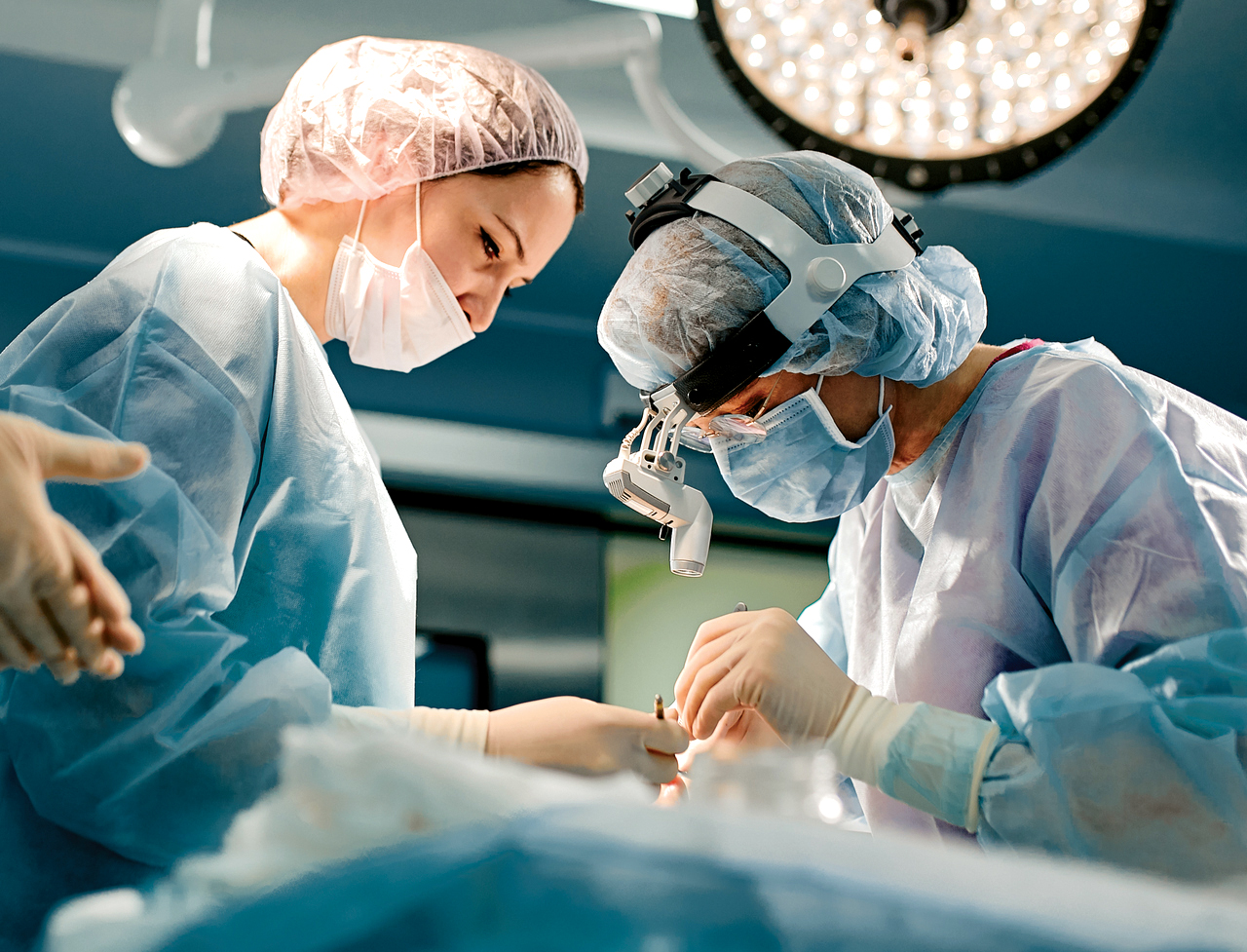
Quality
-

Rural Health Care
-

Surprise Billing
-

Telehealth
-

Volunteers
-
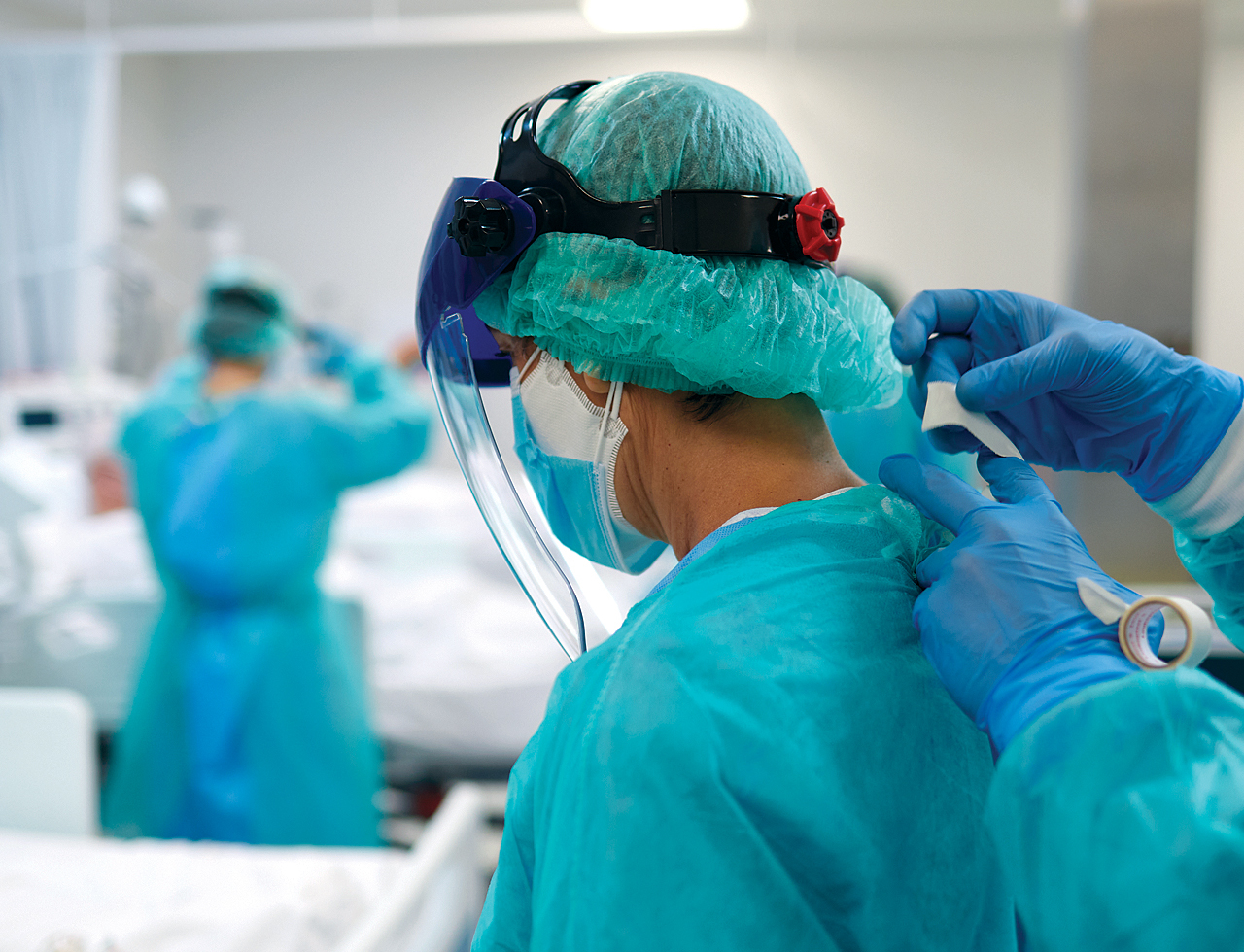
Workforce